How to fix IT Band Syndrome
If you’re an active individual, you may have experienced discomfort or irritation at your IT band a.k.a. the iliotibial band.
IT band syndrome is pain along the outside of the knee that is typically felt while the knee is slightly bent during movement, and can become so bothersome that it sidelines you from activity. It is the second most common cause of knee pain.
Who Is At Risk of IT Band Syndrome?
IT band syndrome typically affects people that run, cycle, hike and participate in sports that require significant power and strength from the legs. Those that experience IT band pain often present with some form of dysfunction with one of the muscles that attach to the IT band – that is, the gluteus medius, gluteus maximus, tensor fasciae latae, or vastus lateralis. Dysfunction in these muscles can include muscle tightness, weakness, and overuse.
What Are the Symptoms of IT Band Pain?
IT band syndrome is felt along the outside of the knee joint. This pain tends to worsen with activity, and ease with rest. IT band pain is sometimes known as “IT band friction” in that clicking may be heard when the knee is moving from a bent to straightening position (flexion into extension). The most intense pain is often present when the knee is bent at 30 degrees (a position typically seen in running). Other symptoms can include: clicking on the outside of the knee; warmth and tenderness to the touch along the outside knee; tension and pain along the hip and thigh.You may notice more prominent IT band syndrome symptoms if you’ve:
What Can Be Done to Address IT Band Pain?
Immediate resting, icing, and stretches are typically prescribed when treating acute IT band syndrome. This may be followed by gradual changes to volumes in training, and specific treatment catered to your needs.Your licensed therapist at Myodetox can provide a thorough assessment to determine what structures and movements may be contributing to your IT band pain. Discomfort and tension along the IT band is often the result of dysfunction of the muscles that attach to it along the hip. In fact, some evidence suggests that IT band pain may be muscle weakness at the hips(1). Your licensed therapist can also help with differential diagnosis of your pain, carefully reviewing other structures that may or may not be contributing to your pain.
Interventions that can help IT band syndrome include:
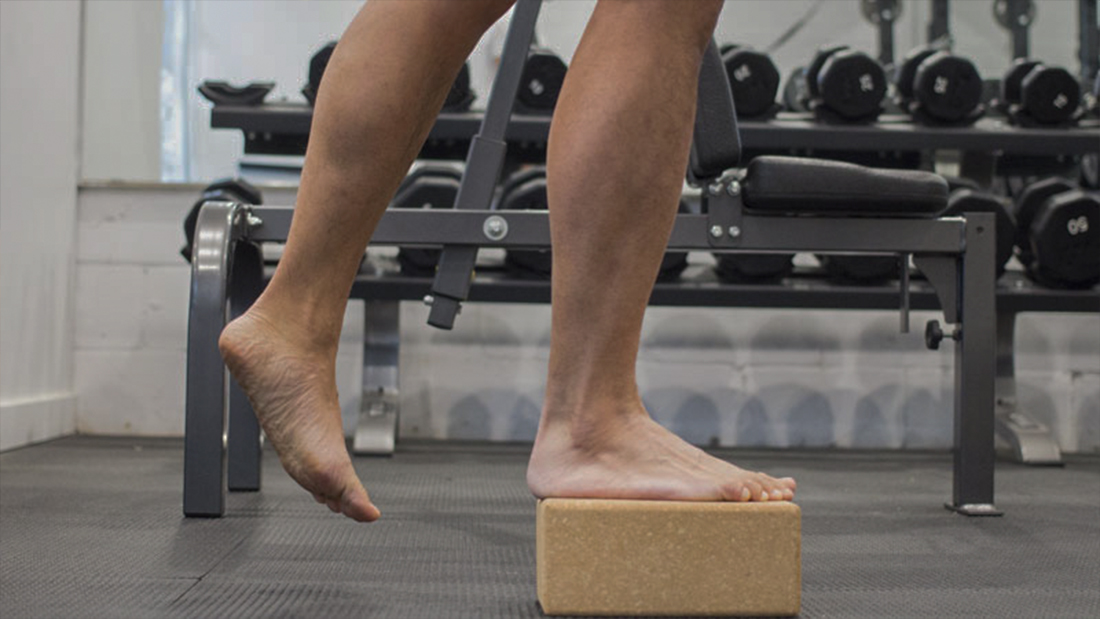
Two Home Exercise Tips:
Click here to watch the video
Click here to watch the video