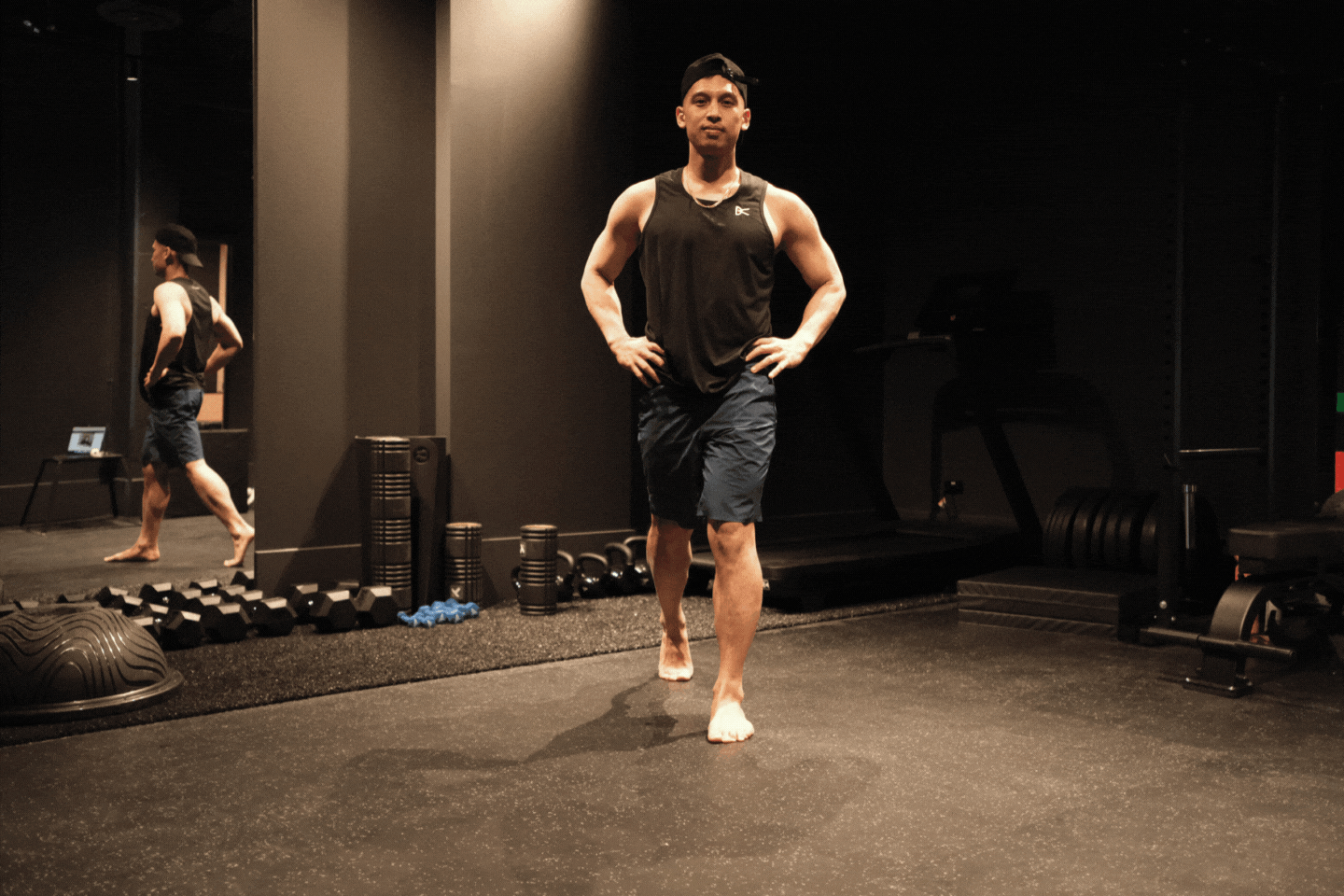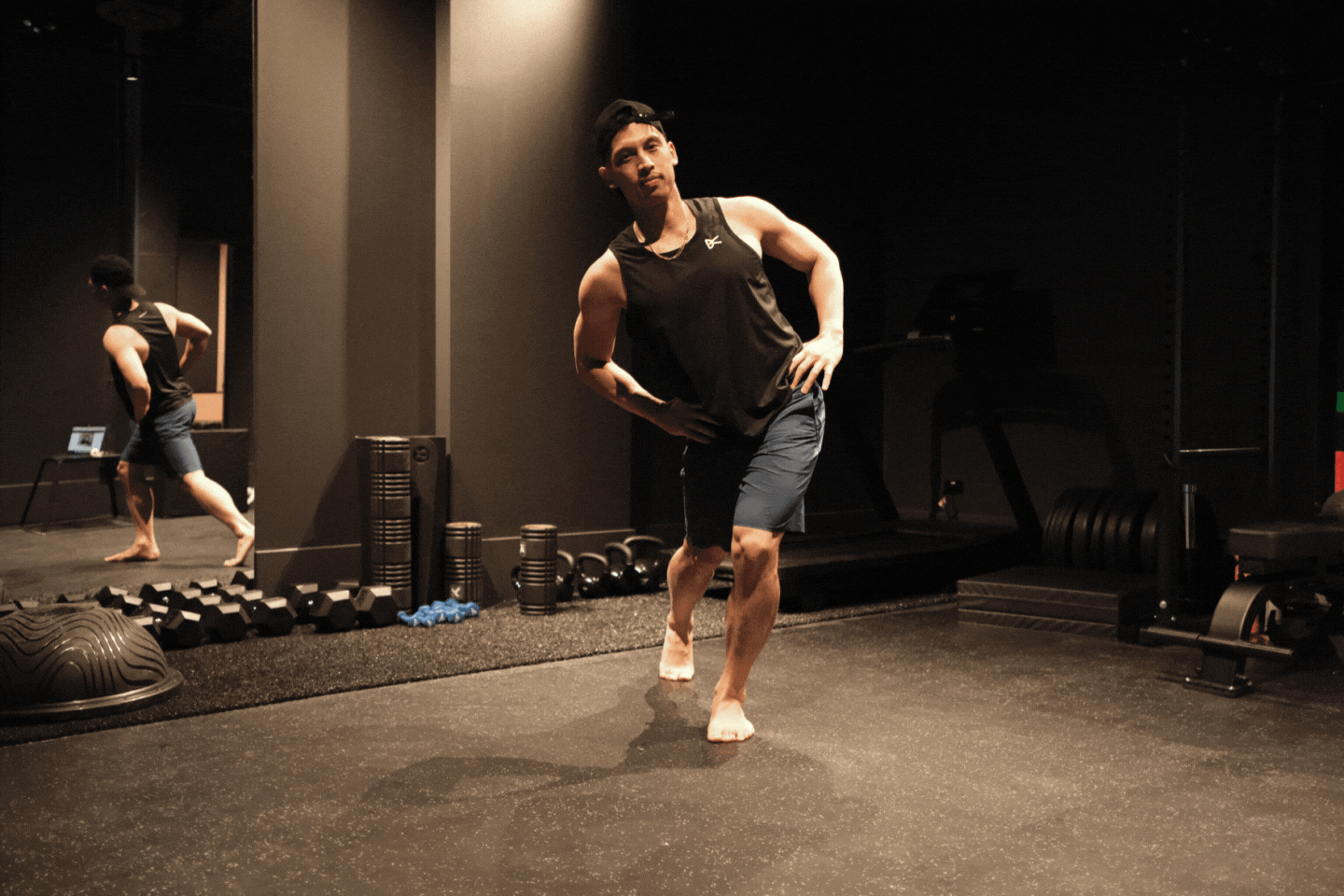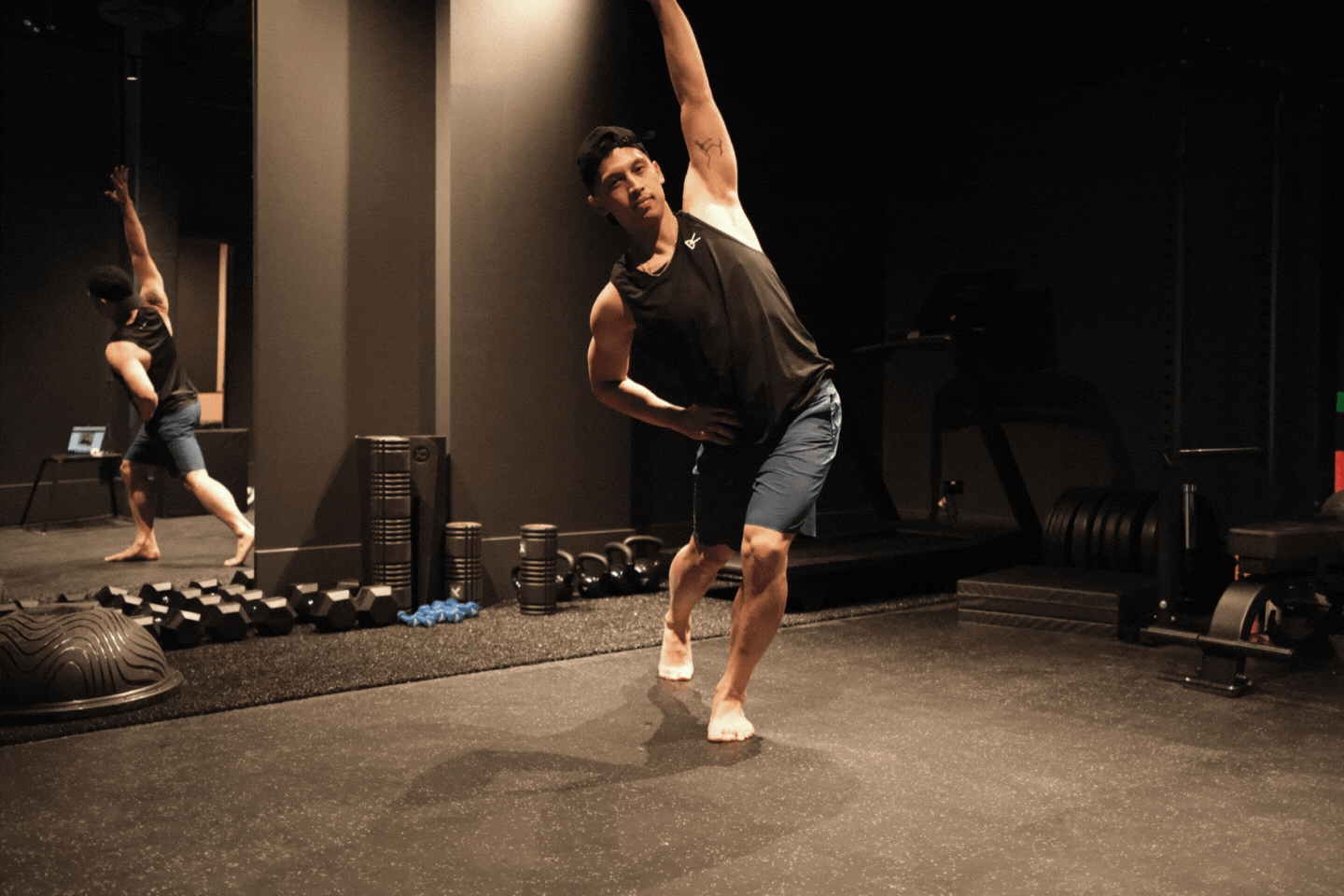Increase Your Mid-Back Mobility With These Three Exercises
The thoracic spine, also known as the middle back, is the middle section of the back, where our ribcage connects and helps protect our organs.
Functional mobility in the middle back (mid-back) is essential. A lack of mid back mobility over time can be a significant factor of improper breathing techniques, neck pain, low back pain, and shoulder pain. Those who are most at risk for losing thoracic motion include office workers, professional drivers, new moms, or anyone sustaining poor postures.Maximizing your mid back mobility is the first step in overcoming mid back stiffness. The more you can build new movements into your daily routine, the sooner you will feel better. The second step is building control in those directions, adding strength and familiarity to those movements.
To help increase the mobility of your mid-back, try these three exercises.
Standing Rib Cage Rotation

Start position Stand in a mini lunge. Raise the arm on the same side as your front leg to shoulder height and the opposite arm straight above your head.
Rotate the ribs as far as you can towards the front leg. Keep legs and arms in the same position.
End position After 3-5 seconds, rotate back to starting position.
Complete 8-10 times on both sides, 2-3 times daily.
Standing Thoracic Extension With Double Arm Reach

Start position Stand in a mini lunge. Arms long by side. Tuck bottom under to limit lower back movement.
End position Raise both arms and lift chest upwards to extend mid back.
Complete 5 times on both sides, 2-3 times daily.
Side Bend Stretch

Start position Stand in a mini lunge. Lace hands behind neck at base of neck, keep elbows wide.
End position Lift one elbow up to the ceiling. Allow ribcage to tilt to one side. Feel stretch between ribs and pelvis.
Complete 5 times on both sides, 2-3 times daily.