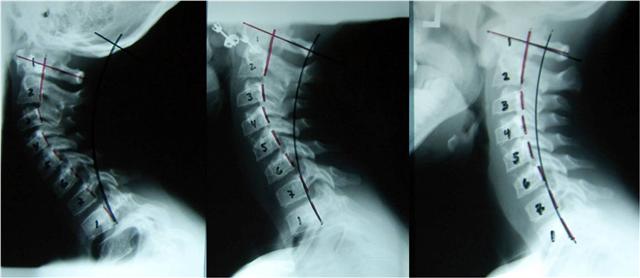
How to Treat a Pinched Nerve in Your Neck
Cervical Radiculopathy Explained
Have you ever had numbness or tingling going down your arms or fingers? You may have experienced cervical radiculopathy, also known as nerve compression or a pinched nerve in your neck. This unassuming injury occurs in nearly 2 out of 1000 people.
What Is A Cervical Radiculopathy?
Cervical radiculopathies are the result of compression and inflammation of a nerve at the neck. There are various conditions that may lead to nerve compression:
Who Gets Nerve Compression?
The population most at risk for developing pinched nerves is the 50+ age. Women are more at risk than men, though the difference is mild.Symptoms Of A Pinched Nerve In Your Neck
The nerves from the neck connect to your trunk, shoulder, arm, hand, and fingers. Symptoms of nerve compression can radiate to any one of those regions:Radicular symptoms like pain and nerve sensations are often felt down the arm. Moving the neck becomes incredibly painful. Performing certain movements may change your symptoms – for better or worse.
Many cases will present with reduced reflexes and muscle weakness. The most common region affected is the C7 nerve root, the C6 nerve root, and the C5 nerve root. Common movements affected by a pinched nerve in your neck are pushing, pulling, and gripping.
Cervical radiculopathies typically occur on one side of the body. If you’re noticing nerve symptoms down both sides, see your physician immediately.
How Do You Treat It?
Treatment of cervical radiculopathy will involve your physician and physical therapist.Your physician can perform tests to identify the cause of your nerve compression. Your physician and physical therapist can perform tests to determine the extent of the compression and provide treatment options such as:
Postural training: nerve compression may be aggravated by a forward head posture. This requires postural awareness, education, and exercises.
Exercise: strength training of the muscle can dramatically improve symptoms.
Check out our IG posts dedicated to neck strengthening.
Manual therapy: traction, myofascial techniques, and joint mobilizations dedicated to improving posture and reducing muscle tension can provide relief.
Check out this post about manual therapy for the neck.
Immobilization: temporarily providing a soft collar to reduce nerve symptoms. Be aware, there is minimal evidence supporting this.
Medication: provided under the guidance of a physician.
Surgery: when conservative management fails, and serious nerve symptoms are present.
There is good news for those with a pinched nerve. Your symptoms will nearly fully resolve in 4-6 months. Up to 90% of people with nerve compression maintain recovery for 4 years. This shows that degenerative changes in the neck do not lead to permanent nerve damage.